1. Introduction to Telemedicine
What is Telemedicine?
Telemedicine refers to the use of digital technology to deliver healthcare services remotely. This includes consultations, diagnoses, and treatment plans conducted over video calls, phone calls, or through secure messaging platforms. It eliminates the need for patients to travel to healthcare facilities, making medical assistance more accessible. As a result, telemedicine has redefined the patient-doctor relationship, offering convenience without compromising care quality.
The Evolution of Telemedicine in Healthcare
Telemedicine began as a means to bridge healthcare gaps in remote areas. Initially, it relied on simple communication tools like telephone consultations. Over time, advancements in technology expanded its capabilities, incorporating video conferencing, electronic health records, and remote diagnostic tools. Today, telemedicine is an integral part of modern healthcare, supported by innovative platforms that deliver high-quality care regardless of location.
Why Telemedicine is Gaining Popularity
The rise of telemedicine can be attributed to its ability to address key healthcare challenges. In an increasingly connected world, patients expect faster, more convenient solutions for their medical needs. Telemedicine meets these demands by reducing wait times, offering flexible scheduling, and ensuring care is accessible from home. The COVID-19 pandemic further accelerated its adoption, highlighting the importance of virtual care during emergencies.
Moreover, telemedicine’s adaptability to diverse medical fields such as primary care, mental health, and chronic disease management makes it invaluable. It enhances patient outcomes while reducing costs, making it a preferred option for individuals and healthcare systems alike.
Telemedicine represents the future of healthcare, with its potential to transform how care is delivered across the globe. Its role in creating a more inclusive and efficient healthcare ecosystem cannot be overstated.
Affiliate Disclaimer
This blog post may include links to affiliate sites. If you click on an affiliate link and make a purchase, we may earn a small commission or receive other compensation at no extra cost to you. Please note that many of the links on our site are affiliate links. Our use of these links does not impact the products, services, or websites we recommend to you. This disclaimer covers all forms of communication with you, including our website, email, phone, social media, products, and other platforms.
Amazon Affiliate Disclaimer
We participate in the Amazon Services LLC Associates Program, an affiliate marketing program that allows us to earn fees by linking to Amazon.com and its affiliated sites. If you click on an Amazon affiliate link on our site and make a purchase, we may receive a small commission at no additional cost to you.
2. Benefits of Telemedicine
Improved Access to Healthcare Anywhere
Telemedicine has revolutionized the way patients access healthcare by breaking down geographical barriers. For individuals in remote or rural areas, reaching a healthcare provider can be challenging due to distance, lack of transportation, or limited local resources. Telemedicine bridges this gap, offering consultations and care from specialists without the need for travel. This accessibility is particularly critical for those with mobility issues or chronic conditions requiring frequent check-ins. By enabling care from virtually anywhere, telemedicine ensures that healthcare is no longer restricted by location.

Cost-Effectiveness for Patients and Providers
One of the most compelling advantages of telemedicine is its cost-saving potential. For patients, it eliminates expenses associated with travel, childcare, or time off work to attend appointments. Providers, on the other hand, can reduce overhead costs by operating smaller clinics or offering telemedicine services as part of their practice. Additionally, telemedicine often helps prevent unnecessary emergency room visits or hospitalizations by enabling timely intervention for minor or chronic health issues. The financial benefits contribute to its growing popularity among both patients and healthcare professionals.
Enhanced Convenience and Time-Saving
Telemedicine fits seamlessly into busy lifestyles, making healthcare more accessible to individuals with demanding schedules. Traditional in-person appointments often require time-consuming travel and long waits at clinics. With telemedicine, patients can schedule consultations at times that suit them, even during evenings or weekends. This flexibility encourages individuals to seek medical attention promptly, addressing health concerns before they escalate.
For healthcare providers, telemedicine increases efficiency by allowing them to manage their schedules more effectively. This streamlined process benefits both parties, fostering a more productive and stress-free healthcare experience.
Increased Patient Engagement and Monitoring
Telemedicine fosters stronger connections between patients and providers, leading to improved health outcomes. Through regular virtual check-ins and remote monitoring tools, providers can track patients’ progress more closely. For example, wearable devices can collect and transmit real-time health data such as blood pressure, glucose levels, or heart rate, enabling early detection of potential problems.
This consistent engagement empowers patients to take an active role in their healthcare. Telemedicine platforms often include educational resources, reminders, and goal-tracking features that encourage adherence to treatment plans. For chronic conditions such as diabetes or hypertension, this level of monitoring and support is invaluable in maintaining long-term health.
Addressing Public Health Challenges
Telemedicine also plays a crucial role in addressing broader public health challenges. During outbreaks or pandemics, it minimizes the risk of virus transmission by reducing in-person visits. Patients can consult with doctors from the safety of their homes, keeping healthcare facilities reserved for critical cases. This capability highlights telemedicine’s role in creating a safer, more adaptable healthcare system that meets the needs of diverse populations.
In summary, telemedicine’s benefits are multifaceted, ranging from increased accessibility and cost-effectiveness to enhanced patient engagement. Its potential to transform healthcare delivery is undeniable, making it a vital component of the modern healthcare landscape.
3. Key Applications of Telemedicine
Primary Care and Routine Consultations
Telemedicine has become an essential tool for primary care, allowing patients to consult with doctors for routine health concerns without needing to visit a clinic. Common issues such as colds, flu, minor infections, or skin conditions can be effectively addressed through virtual consultations. Doctors can diagnose symptoms, provide medical advice, and even prescribe medications through secure telemedicine platforms. This approach reduces the strain on healthcare facilities while ensuring patients receive timely care for non-emergency issues.
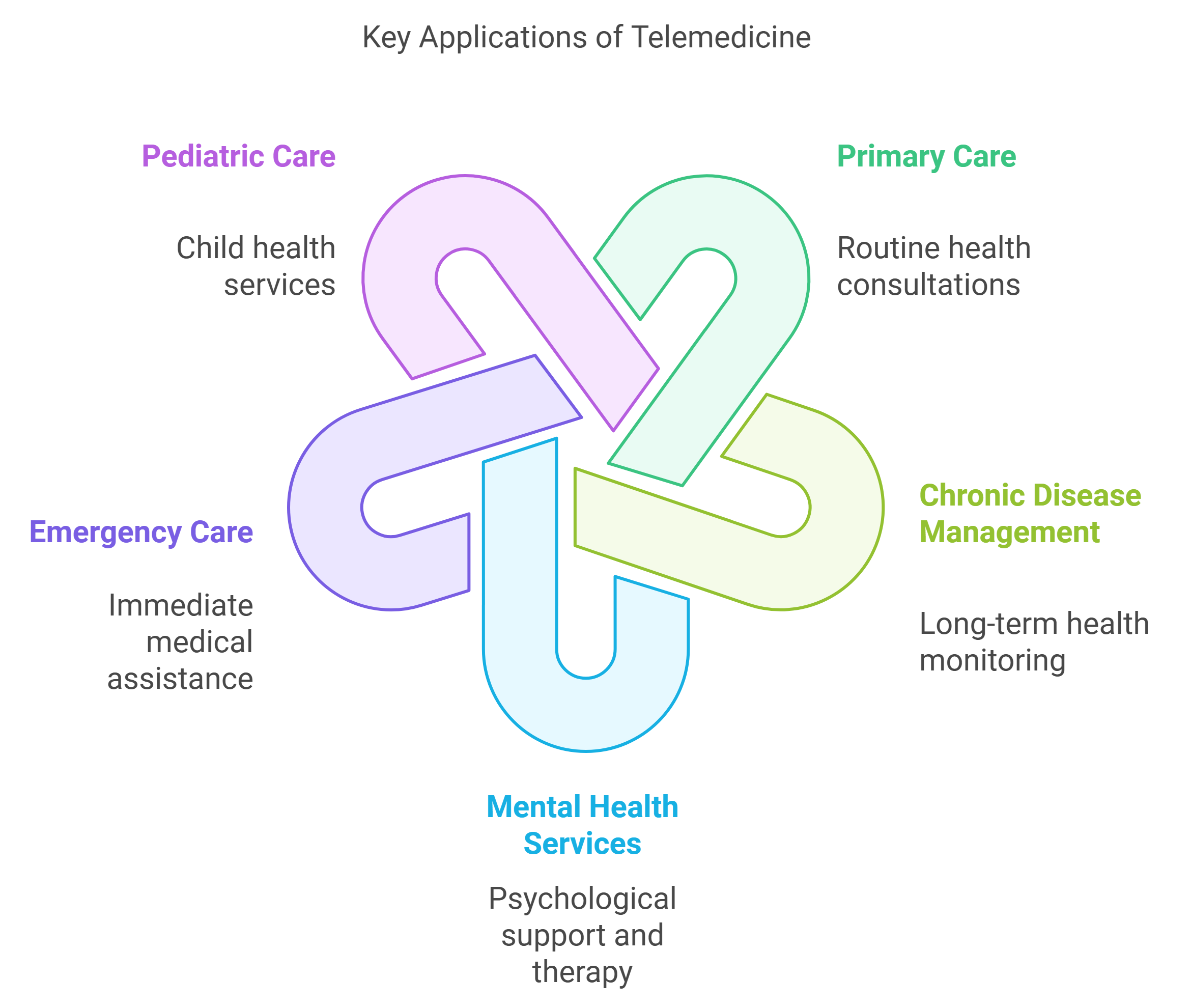
Chronic Disease Management
Managing chronic conditions such as diabetes, hypertension, or asthma often requires regular monitoring and consistent communication with healthcare providers. Telemedicine simplifies this process by offering remote check-ins and virtual follow-ups. Patients can share real-time data from wearable devices, such as blood sugar levels or blood pressure readings, directly with their providers.
Telemedicine also supports personalized care plans, allowing doctors to adjust treatments based on the latest data. This ongoing interaction improves outcomes, reduces hospital readmissions, and empowers patients to manage their health actively.
Mental Health Services via Telemedicine
The demand for accessible mental health services has grown significantly, and telemedicine has stepped in to fill this need. Through video conferencing or secure messaging, patients can access therapy and counseling sessions from the comfort of their homes. This approach eliminates common barriers to mental health care, such as stigma, long wait times, or limited availability of providers in rural areas.
Telemedicine’s flexibility is particularly beneficial for mental health, as it allows patients to connect with therapists at convenient times. Whether for anxiety, depression, or more severe disorders, telemedicine ensures that mental health care is more inclusive and readily available.
Emergency and Acute Care Support
Telemedicine is also proving invaluable in emergency and acute care situations, where immediate guidance can save lives. For instance, patients experiencing minor injuries or symptoms that may not require a trip to the emergency room can use telemedicine to consult with healthcare professionals. Providers can quickly assess the situation, recommend treatment, or determine if in-person care is necessary.
In rural or underserved areas, telemedicine connects local clinicians with specialists in real-time, enabling faster diagnosis and treatment during critical moments. This application is particularly vital for conditions such as strokes, where rapid intervention can make a significant difference in outcomes.
Pediatric and Family Care
Telemedicine is increasingly popular for pediatric care, providing parents with a convenient way to address their children’s health concerns. From assessing fevers to evaluating minor injuries, telemedicine allows parents to consult with doctors without disrupting their routines.
By addressing diverse healthcare needs, telemedicine ensures that medical care is more accessible, efficient, and tailored to the demands of modern life. Its wide-ranging applications make it a transformative force in healthcare, bridging gaps and improving outcomes for patients across all demographics.
4. Technology Driving Telemedicine
Role of Mobile Devices and Apps
Mobile devices have become indispensable in the rise of telemedicine, enabling patients and healthcare providers to connect instantly. Smartphones and tablets serve as portals for telemedicine apps, offering features like video calls, appointment scheduling, and prescription management. These user-friendly apps provide secure, convenient platforms for patients to access medical care from anywhere.
Beyond consultations, mobile apps are being integrated with health tracking systems, allowing patients to monitor vital signs, manage chronic conditions, and share data directly with their providers. This functionality makes mobile devices a cornerstone of telemedicine, driving its adoption across diverse demographics.

Integration of Artificial Intelligence in Telemedicine
Artificial intelligence (AI) is revolutionizing telemedicine by enhancing diagnostic accuracy and streamlining workflows. AI-powered tools can analyze patient data, such as symptoms, medical history, or test results, to assist doctors in making informed decisions.
Chatbots and virtual assistants powered by AI can provide initial triage, answer patient queries, and guide them to appropriate care. Additionally, AI algorithms can identify patterns in large datasets, predict potential health issues, and recommend preventive measures. By incorporating AI, telemedicine is becoming more efficient and effective, improving both patient and provider experiences.
Wearable Devices and Remote Monitoring Tools
Wearable devices are a game-changer for telemedicine, enabling continuous monitoring of a patient’s health. Devices like smartwatches, fitness trackers, and medical-grade sensors collect data on heart rate, blood pressure, oxygen levels, and more. This real-time data can be shared with healthcare providers, allowing them to track progress, detect anomalies, and adjust treatment plans remotely.
Remote monitoring tools are particularly beneficial for patients with chronic conditions such as diabetes, cardiovascular diseases, or respiratory disorders. These tools empower patients to stay proactive about their health while ensuring their providers have up-to-date information for better decision-making.
Importance of Secure Communication Platforms
Telemedicine relies on secure communication platforms to ensure patient privacy and confidentiality. Video conferencing tools and messaging systems must comply with strict data protection regulations, such as HIPAA, in the United States. Encryption and secure data storage are essential features of these platforms, safeguarding sensitive medical information from cyber threats.
In addition to security, these platforms offer seamless integration with electronic health records (EHRs), ensuring providers can access and update patient information in real time. This connectivity improves coordination among healthcare teams and enhances the overall quality of care delivered through telemedicine.
Advancing Connectivity for Seamless Care
The effectiveness of telemedicine depends on reliable internet connectivity. Advances in broadband networks and the rollout of 5G technology have greatly improved the quality of virtual consultations, reducing delays and ensuring clear communication. As connectivity improves worldwide, telemedicine will continue to expand its reach, bringing high-quality care to underserved regions.
Technology is the backbone of telemedicine, driving innovation and making healthcare more accessible, efficient, and personalized. With continuous advancements, telemedicine is poised to redefine the delivery of medical services globally.
5. Challenges Facing Telemedicine Adoption
Regulatory and Licensing Barriers
One of the most significant hurdles for telemedicine adoption is navigating complex regulatory and licensing requirements. Healthcare regulations often vary by country, state, or region, creating challenges for providers who want to deliver cross-border services. For instance, many regions require doctors to be licensed in the patient’s location, complicating the expansion of telemedicine services.
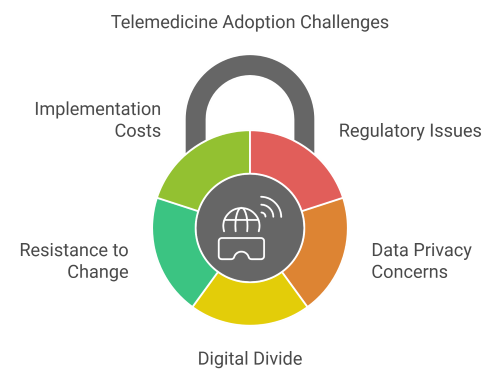
These restrictions can hinder the potential of telemedicine to provide universal access to care, especially in underserved areas. Addressing these regulatory inconsistencies is essential for enabling seamless, widespread telemedicine adoption. Efforts are being made to standardize policies, but progress remains slow, limiting the growth of this transformative healthcare model.
Data Privacy and Security Concerns
With telemedicine relying heavily on digital platforms, data privacy and security are paramount concerns. Patients must share sensitive health information during virtual consultations, which makes these platforms a prime target for cyberattacks. Breaches can lead to the exposure of confidential medical records, undermining trust in telemedicine systems.
Ensuring compliance with stringent data protection laws, such as HIPAA in the United States and GDPR in Europe, is critical for telemedicine providers. Encryption, secure authentication processes, and robust cybersecurity measures are necessary to safeguard patient data. However, implementing these solutions requires significant investment and expertise, which can be a barrier for smaller providers.
Digital Divide: Accessibility Issues in Rural Areas
While telemedicine has the potential to improve access to healthcare, the digital divide poses a major challenge. Rural areas often lack reliable internet connectivity and modern infrastructure, making it difficult for residents to use telemedicine services effectively. Additionally, some individuals may not have access to smartphones, tablets, or computers needed for virtual consultations.
This disparity also affects older adults or those who are less tech-savvy, as they may struggle to navigate telemedicine platforms. Bridging the digital divide requires investments in broadband expansion, affordable technology, and user-friendly interfaces. Without these efforts, telemedicine risks leaving behind the very populations it aims to serve.
Resistance to Change Among Providers and Patients
Adopting telemedicine requires a shift in how healthcare is delivered and received, and not everyone is ready for this change. Some healthcare providers are hesitant to incorporate telemedicine due to concerns about its effectiveness compared to in-person care. Others may lack the technical training or resources needed to adopt telemedicine tools.
Similarly, patients accustomed to traditional consultations may feel uneasy about virtual care. They might question the quality of care or worry about the lack of personal interaction. Building trust through education, training, and positive experiences is essential to overcoming this resistance and ensuring telemedicine becomes a widely accepted option.
Cost of Implementation for Providers
For healthcare providers, adopting telemedicine can be a costly endeavor. Developing secure, compliant platforms, training staff, and integrating telemedicine with existing systems require significant investment. Smaller practices and healthcare facilities may struggle to afford these expenses, limiting their ability to offer telemedicine services.
Despite these challenges, telemedicine remains a powerful tool for transforming healthcare. Addressing these barriers through regulatory reform, improved infrastructure, and patient education will be key to unlocking its full potential.
6. The Future of Telemedicine in Healthcare
Expansion into Specialized Healthcare Fields
The future of telemedicine lies in its ability to serve a broader range of specialized healthcare needs. Beyond routine consultations and primary care, telemedicine is making inroads into fields such as dermatology, cardiology, and oncology. Dermatologists can evaluate skin conditions through high-resolution images, while cardiologists can monitor heart conditions with real-time data from wearable devices.

In oncology, telemedicine is being used to provide follow-up care, manage treatment side effects, and even conduct virtual tumor board meetings for collaborative decision-making. As technology advances, more specialized areas of medicine will adopt telemedicine, making it a cornerstone of comprehensive healthcare delivery.
Role of 5G and Advanced Connectivity in Telemedicine Growth
The rollout of 5G technology is set to revolutionize telemedicine by addressing one of its most significant challenges—reliable and fast connectivity. With higher bandwidth and lower latency, 5G enables smoother video consultations, instant data sharing, and the integration of advanced technologies like augmented reality (AR) and virtual reality (VR).
For instance, surgeons can use VR tools powered by 5G to guide remote procedures or provide consultations during critical emergencies. Similarly, rural clinics can connect to specialists in real time, offering advanced care to underserved populations. As 5G networks become more widespread, telemedicine will become more efficient and accessible, even in areas that previously struggled with connectivity issues.
Predictions for Global Adoption Trends
Globally, the adoption of telemedicine is expected to accelerate, driven by increasing healthcare demands, technological advancements, and changing patient expectations. Developing countries are likely to benefit the most as telemedicine bridges healthcare access gaps in remote regions. Governments and private organizations are investing in infrastructure and training to support this growth, making telemedicine a vital part of public health initiatives.
Artificial intelligence and machine learning are also predicted to play a larger role in telemedicine’s future. These technologies will enhance diagnostic accuracy, automate administrative tasks, and provide personalized care recommendations. Furthermore, blockchain technology is poised to improve data security and interoperability, addressing key concerns around patient privacy.
Integration with Preventive and Predictive Medicine
The future of telemedicine will extend beyond treatment to include preventive and predictive care. Telemedicine platforms will leverage big data to analyze health trends, predict potential health risks, and recommend proactive interventions. For example, wearable devices can alert patients and providers to early signs of chronic conditions, enabling timely action to prevent complications.
Telemedicine will also integrate with population health management programs, using data analytics to improve health outcomes on a larger scale. By focusing on prevention and prediction, telemedicine will shift healthcare from reactive to proactive, fostering healthier communities worldwide.
Telemedicine as a Global Standard
As telemedicine continues to evolve, it is expected to become a global standard for healthcare delivery. Its ability to adapt to diverse needs, reduce costs, and improve outcomes ensures its longevity and growth. With innovations in technology and increased acceptance by providers and patients alike, telemedicine is poised to redefine healthcare for future generations.
7. Conclusion
Telemedicine as a Game-Changer in Healthcare
Telemedicine has proven to be a transformative force in healthcare, breaking down barriers to access and introducing innovative solutions to modern challenges. By enabling patients to connect with providers remotely, it has redefined convenience and efficiency in medical care. Whether through routine consultations, chronic disease management, or mental health services, telemedicine ensures that quality care is available to individuals regardless of their location.
Telemedicine’s benefits extend beyond accessibility. It reduces healthcare costs, empowers patients to take charge of their health, and fosters stronger relationships between providers and patients. Technology continues to enhance its capabilities, with advancements like AI, wearable devices, and 5G connectivity expanding its potential further.
As telemedicine becomes more integrated into healthcare systems worldwide, its ability to address public health challenges and deliver personalized, preventive care will only grow. However, overcoming barriers such as regulatory complexities, data security, and the digital divide is crucial to unlocking its full potential.
In a rapidly evolving healthcare landscape, telemedicine stands out as a game-changer, offering a future where high-quality, patient-centered care is accessible to everyone, anywhere in the world. Its journey is just beginning, with endless opportunities ahead.
Top 7 FAQs for Telemedicine Transforming Healthcare Anywhere
- What is telemedicine, and how does it work?
Telemedicine is the remote delivery of healthcare services using technology like video calls, phone consultations, or mobile apps. Patients connect with healthcare providers to discuss symptoms, receive diagnoses, and get treatment plans without visiting a clinic in person. - What types of healthcare services can telemedicine provide?
Telemedicine supports various services, including routine consultations, chronic disease management, mental health therapy, dermatology assessments, and even post-surgical follow-ups. In some cases, it also aids in emergency care by providing quick access to specialists. - Is telemedicine as effective as in-person visits?
For many conditions and routine care, telemedicine is highly effective, offering the same quality of care as in-person visits. However, for emergencies or cases requiring physical examination, in-person care might be necessary. - Who can use telemedicine?
Telemedicine is accessible to anyone with a stable internet connection and a compatible device. It is especially beneficial for individuals in remote areas, those with mobility issues, or patients with busy schedules. - Does insurance cover telemedicine?
Many insurance providers now cover telemedicine services, but the extent of coverage varies. It’s best to check with your provider to understand the details. - How secure is telemedicine for sharing personal health information?
Telemedicine platforms are designed to comply with privacy laws like HIPAA, using encryption and secure communication to protect patient data. Always verify the security features of the platform being used. - What equipment do I need for a telemedicine appointment?
Typically, you need a smartphone, tablet, or computer with a camera, microphone, and stable internet. Many telemedicine platforms also offer apps for seamless access.


